Introduction
A boutonnière deformity can impact the index, middle, ring, and little fingers, often stemming from tendon injury at the middle joint (the proximal interphalangeal, or PIP joint). Causes include trauma like lacerations or dislocations or soft tissue damage from conditions like rheumatoid arthritis. This leads to a flexed PIP joint and a hyperextended fingertip. Prompt treatment can reverse traumatic cases, but chronic deformities or those from rheumatologic conditions may worsen, potentially causing permanent deformity and impaired finger function.

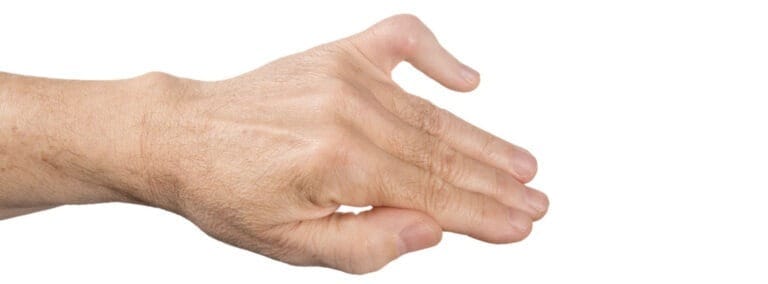
In a Boutonnière deformity, the affected finger exhibits a distinct shape: the middle joint remains bent, unable to straighten, while the fingertip bends backwards.
Anatomy
Multiple tendons in the fingers collaborate to facilitate bending and straightening movements. These tendons traverse the underside, sides, and top of the finger.
A significant portion of the tendon situated on the finger’s top surface (known as the central slip) connects to the middle bone of the finger (the middle phalanx) and functions to straighten the middle (PIP) joint.
Cause
Boutonnière deformity typically arises from trauma, which can occur in several ways:
- A forceful impact on the top (dorsal) side of a finger’s bent (flexed) middle joint leads to either central slip rupture or fracture where the central slip attaches to the middle phalanx bone.
- Dislocation of the middle phalanx towards the finger’s bottom, resulting in central slip detachment from the bone.
- Lacerations on the finger’s top cause central slip severance, resembling a buttonhole (“boutonnière” in French), hence the name. Occasionally, the bone may protrude through the opening.
Additionally, autoimmune arthritis, such as rheumatoid arthritis, can also contribute to boutonnière deformities by deteriorating soft tissues and weakening the central slip.
Symptoms of Boutonnière Deformity
Manifestations of boutonnière deformity can arise either immediately following a finger injury or several weeks later:
- The inability to straighten the finger at the middle (PIP) joint and difficulty bending the fingertip, resulting in the distinctive deformity.
- Swelling and pain develop over the top of the PIP joint.
Diagnosis of Boutonnière Deformity
When suspecting a boutonnière deformity, seeking medical attention is crucial for accurate diagnosis and appropriate treatment. During your doctor’s visit, they will:
- Conduct a thorough examination of the fingers and hand.
- Ask you to attempt straightening the affected finger and bending the fingertip.
- Consider ordering X-rays to identify any potential fractures involving the central slip of the tendon.
- Potentially perform the Elson Test, a specialised assessment for detecting central slip insufficiency.
This involves bending the PIP joint of the affected finger to 90° and asking you to attempt straightening it against resistance while the doctor assesses fingertip mobility.
Restricted movement during this test indicates a central slip injury, raising concerns about the development of a boutonnière deformity.
Nonsurgical Treatment for Boutonnière Deformity
Prompt treatment is essential for boutonnière deformity resulting from traumatic injury to preserve full finger motion.
Nonsurgical approaches are typically favoured and may involve:
Splinting:
A splint is applied to the middle joint of the finger to straighten it, preventing tendon separation during healing.
This also permits the bending of the fingertip. While wearing the splint, it’s important to exercise bending the fingertip to maintain proper tendon positioning.
Continuous splint wear for the recommended duration, usually 6 to 8 weeks, is crucial.
Accidental bending of the finger at the middle joint outside of the splint during treatment can reverse progress. Following the immobilisation period, wearing the splint at night may still be necessary.
Rehabilitation and Protection
Your physician may prescribe stretching exercises to enhance finger strength and flexibility. During splint wear, exercises will target the DIP joint (the finger’s last joint), requiring regular daily bending.
Protective splinting or taping may be necessary for several weeks post-splint removal for sports enthusiasts.
Individuals with boutonnière deformity due to arthritis may receive treatment such as oral medications or corticosteroid injections combined with splinting.
Surgical Options for Boutonnière Deformity
While nonsurgical approaches are typically preferred for boutonnière deformity, surgery may be necessary under certain circumstances, such as:
- Deformity resulting from rheumatoid arthritis
- Severed tendon
- Displaced large bone fragment
- Lack of improvement with splinting
Surgical intervention aims to alleviate pain and enhance function, although complete correction and restoration of normal finger appearance may not always be achievable. Delaying treatment beyond 3 weeks can complicate management significantly.
Surgical techniques may involve:
- Realigning a dislocated PIP joint and inserting a temporary pin to maintain straightness for 6 to 8 weeks
- Reattaching an avulsed central slip to the middle phalanx bone using an anchor
- Repairing a lacerated central slip
- Fixing a broken piece of the middle phalanx with attached central slip using pins or plates/screws
- Utilising a tendon slip as a graft to create a new central slip
- Releasing the terminal tendon where it connects to the distal phalanx to alleviate hyperextension of the DIP joint
Outcomes
Success in managing boutonnière deformity hinges on various factors including treatment modality, timeliness, and individual anatomical and injury considerations.
Early intervention yields superior results; therefore, prompt consultation with a hand surgeon upon suspicion of a finger injury is crucial.
Traumatic injuries addressed either nonsurgically or surgically within 3 weeks tend to have favourable outcomes.
Chronic injuries and deformities from rheumatologic conditions pose greater challenges and may yield unpredictable results.